Platelet-rich plasma (PRP) therapy is an advanced regenerative treatment that uses a patient’s own blood to promote healing, reduce inflammation, and support tissue repair. Increasingly used in musculoskeletal and aesthetic medicine, PRP reflects a shift toward treatments that work with the body’s natural biology rather than masking symptoms.
What is PRP Therapy?
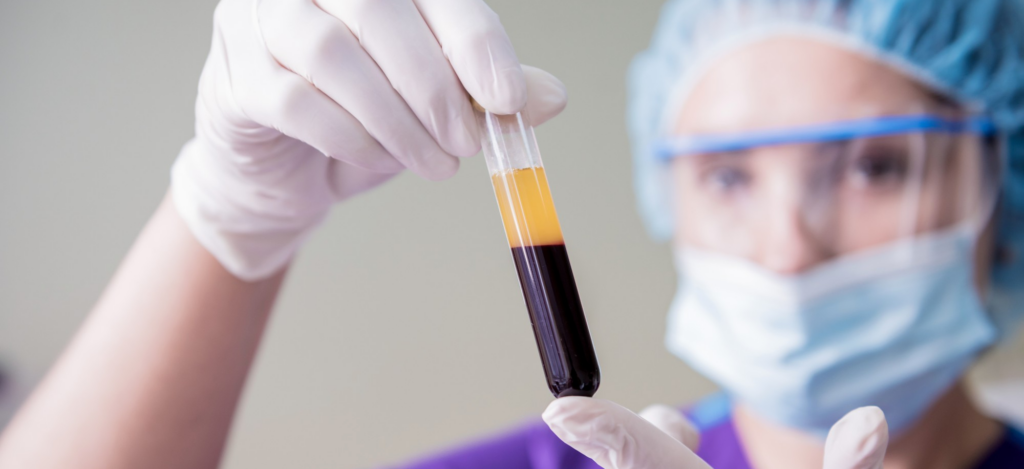
PRP is created by drawing a small sample of a patient’s blood and processing it in a centrifuge to concentrate platelets within the plasma. These platelets are rich in growth factors—biologically active proteins that play a key role in tissue repair and regeneration.
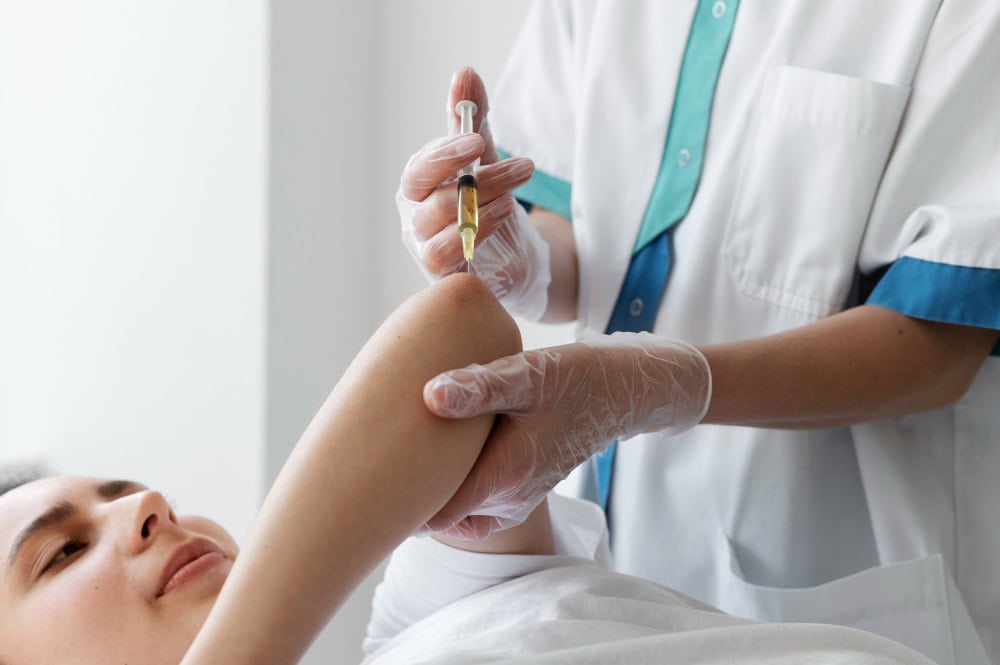
Once prepared, the platelet-rich plasma is injected into the targeted area, such as a joint, tendon, or skin. The goal is to deliver a high concentration of healing factors directly where the body needs them, potentially accelerating recovery and improving tissue quality.
The History of PRP
The origins of PRP therapy date back several decades and are rooted in hematology. In the 1960s and 1970s, platelet concentrates were first used to treat patients with low platelet counts (thrombocytopenia).
By the 1980s and 1990s, PRP began to be used in surgical fields such as maxillofacial and plastic surgery to enhance healing.
Over time, its applications expanded into orthopedics, sports medicine, and dermatology. Today, PRP is considered one of the key therapies in regenerative medicine, with ongoing research exploring its role across multiple medical specialties.
Common Uses of PRP Therapy
PRP therapy is used in a wide range of clinical settings, particularly where tissue healing is a primary goal. It is commonly applied in musculoskeletal medicine for tendon injuries, ligament strains, and joint conditions such as osteoarthritis, where it may help reduce pain and improve function.
It is also used to support post-injury or post-surgical healing, as well as in aesthetic medicine for skin rejuvenation, scar improvement, and hair restoration. In these contexts, PRP works by stimulating collagen production, improving blood supply, and enhancing tissue regeneration.
Benefits of PRP Therapy

- Uses the patient’s own biological material, reducing the risk of allergic reactions
- Targets the underlying healing process, rather than only masking symptoms
- Minimally invasive, with little downtime compared to surgery
- Versatile applications, from joint care to skin and hair treatments
- Can be combined with other therapies, including physiotherapy or regenerative treatments
Potential Risks and Limitations
PRP therapy is generally considered safe, but it is important to understand its limitations. Because it uses the patient’s own blood, the risk of serious adverse reactions is low; however, mild side effects such as soreness, bruising, or swelling at the injection site can occur.
Less commonly, risks may include infection, bleeding, or tissue irritation. As with any injection-based procedure, proper technique and sterile conditions are essential.
A key limitation of PRP is that results can vary between patients. Factors such as age, overall health, severity of the condition, and the specific preparation technique can all influence outcomes. In addition, PRP typically requires a series of treatments, and improvements may take several weeks to become noticeable.
Current Evidence and Effectiveness
The scientific evidence supporting PRP therapy continues to evolve. Research suggests that PRP may enhance healing by delivering a high concentration of growth factors that stimulate tissue repair and regeneration.
In musculoskeletal conditions such as early osteoarthritis, several studies have shown improvements in pain and function, particularly in younger patients or those with less advanced disease.
Is PRP Therapy Right for You?
PRP therapy may be appropriate for patients seeking a non-surgical approach to managing pain, improving function, or enhancing tissue healing. It is often considered when conventional treatments have not provided sufficient relief or when patients wish to explore regenerative options.
A thorough medical assessment is essential to determine whether PRP is suitable, as well as to ensure that it is integrated effectively into a broader care strategy tailored to the individual.
Key Takeaways
- PRP therapy uses concentrated platelets from your own blood to promote healing
- It has a long history evolving from hematology to modern regenerative medicine
- It is commonly used for joint pain, injuries, skin rejuvenation, and hair restoration
- Evidence is promising but variable, with best results in selected patients
- Treatment should be guided by careful medical evaluation and realistic expectations

